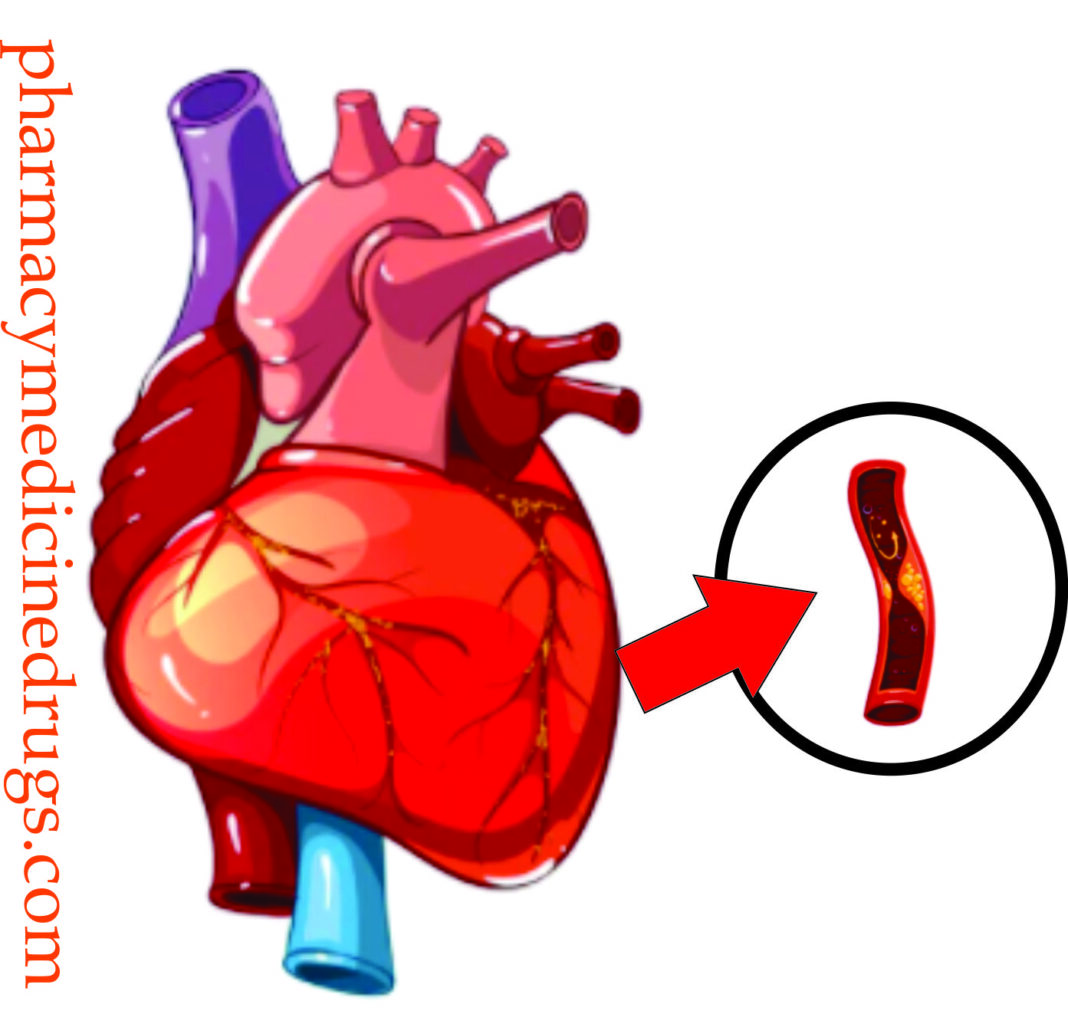
Ischaemic heart disease (IHD) | What Does Ischaemic Heart Disease Mean nhs | What Causes It ?
Ischaemic heart disease (IHD) is defined as ‘acute or chronic form of a cardiac disability
arising from imbalance between the myocardial supply and demand of oxygenated blood’.
The alternate term coronary artery disease (CAD) is used synonymously with IHD. Depending on the rate and severity of coronary artery narrowing and the myocardial response, one of four syndromes may develop.
- Angina pectoris (Chest pain),
- Acute myocardial infarction,
- Chronic ischemic heart disease with congestive heart failure,
- Sudden cardiac death.
Etiology of Ischaemic heart disease (IHD)
The most common cause of ischemic heart disease is a reduction in coronary arterial blood supply due to atherosclerosis of the coronary arteries. Factors that contribute to the development of ischaemic heart disease are similar to those responsible for atherosclerosis in general, and include: Hypertension, diabetes mellitus, smoking, high cholesterol, high levels of low density lipoprotein, and genetic factors and non-atherosclerotic causes are vasospasm, coronary artery stenosis, inflammation of coronary arteries, thrombotic disease, trauma, aneurysms and compression.
Pathogenesis of Ischaemic heart disease (IHD)
Symptomatic ischemic heart disease is typically associated with a critical stenosis, defined as a 75% or greater reduction in the lumen of one or more coronary arteries by atherosclerotic plaque. With this level of fixed obstruction, the augmented coronary
blood follow that may occur as a result of compensatory coronary vasodilation is
insufficient to meet even moderate increase in myocardial oxygen demand. In addition to chronic, fixed atherosclerotic plaques, various superimposed lesions also play an
important role in the development of myocardial ischemia. These include —
- Acute changes in the morphology of chronic atherosclerotic plagues include fissuring, haemorrhage into the plaque, and plaque rupture with embolization of
atheromataous debris into distal coronary vessels. In addition to causing enlargement of the plaque, local disruption of plaque increases the risk of platelet aggregation and thrombosis at the site. - Local plated aggregation in the coronary arteries has been documented in patients with unstable angina pectoris and in patients who undergo sudden cardiac death. Both mechanical occlusion of small blood vessels by small platelet aggregates and coronary vasospasm induced by mediators released from the platelet aggregates may contribute to myocardial ischemia.
- Coronary artery thrombosis is almost always associated with a severe atherosclerotic plaque. Local disruption of atheromataous plaques plays an important role in the development of thrombi by exposing thrombogenic, lipid rich plaque debris to the blood. Thrombi are identified most often in patients who have suffered a myocardial infarct involving the full thickness of the myocardium although they may also occur in patients with other clinical manifestations of cardiac ischemia, such as unstable angina pectoris.
- Coronary artery spasm usually occurs in patients with at least some pre-existing atherosclerosis. It has been associated with one particular type of angina pectoris, termed Prinzmental’s (variant) angina. At the site of plaque disruption, it may be induced by the release of vasospastic mediators such as thromboxane A2 by platelet aggregates. Endothelial dysfunction may also precipitate vasospasm by reduced elaboration of endothelial cell derived relaxing factors. Increased sympathetic activity and smoking have also been implicated.
The process other than atherosclerosis or its complications may compromise blood flow through the coronary arteries such as vasospasm, coronary artery stenosis, inflammation of coronary arteries, thrombotic disease, trauma, aneurysms and compression etc. In addition to factors that compromise coronary blood flow, increased myocardial demand may also contribute the development of myocardial ischemia. This may occur with left ventricular myocardial hypertrophy, as well as other conditions that place an increased demand on the heart such as hypertension and diseases of the heart valves.