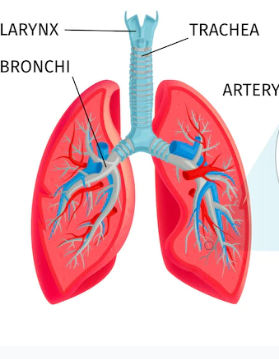
Chronic Obstructive Airways Diseases | Diagnosis Of (COPD)
The symptoms and signs of respiratory failure are not specific. Rather, they depend
on what is causing the failure and on the patient’s condition before it developed.
Physical Examination
It includes history of duration of fever, cough and sputum. Other signs include open mouth respiration, sweating, clicking of tongue etc. Headache, confusion and impaired consciousness may result from high levels of carbon dioxide. Cyanosis may result from low level of oxygen.
Lab Tests:
Arterial blood gas analysis: A test using blood from an artery in wrist can measure oxygen level. A low level of oxygen or a high level of carbon dioxide in the blood (or both) is a possible sign of respiratory failure. Other types of blood tests can check for signs of infection or anemia.
Complete blood count (CBC): Anaemia can contribute to tissue hypoxia; polycythaemia may indicate chronic hypoxaemic respiratory failure. Renal function tests and Liverv function tests: It may provide clues to the etiology or identify complications associated with respiratory failure. Abnormalities in electrolytes such as potassium, magnesium, and phosphate may aggravate respiratory failure and other organ dysfunction.
Serum creatine kinase and troponin I: To help exclude recent myocardial infarction. Elevated creatine kinase may also indicate myositis.
Thyroid function tests: Hypothyroidism may cause chronic hypercapnic respiratory
failure.
Spirometry: It is useful in the evaluation of chronic respiratory failure.
Heart tests: The signs and symptoms of respiratory failure are similar to those of
certain heart problems.
Echocardiography: If a cardiac cause of acute respiratory failure is suspected.
Pulmonary function tests: These tests are useful in the evaluation of chronic respiratory failure.
ECG: To evaluate a cardiovascular cause; it may also detect dysrhythmias resulting from severe hypoxaemia or acidosis.
Right heart catheterization: It should be considered if there is uncertainty about
cardiac function, adequacy of volume replacement, and systemic oxygen delivery.
Imaging Tests:
Chest X-ray: A chest X-ray can reveal, which parts of lungs have fluid in them and whether heart is enlarged.
Computerized tomography (CT): CT scans can provide detailed information about the structures within the heart and lungs.
Treatment For Chronic Obstructive Airways Diseases (COPD)
The goals of treatment for respiratory failure are to increase oxygenation and improve ventilation. Treatment depends on the severity of the respiratory failure and the cause. Acute respiratory failure treatment will address the underlying cause and include ventilation and oxygenation as needed. Exacerbation of chronic respiratory failure by infection may require hospitalization, and treatment for (copd)may include oxygenation and ventilator support. Bronchodilators may improve airway patency. Multiple options are available for the treatment of respiratory failure. Examples include:
- Antibiotics to prevent and treat respiratory infections.
- Bi-level positive airway pressure (BiPAP).
- Bronchodilators, like anticholinergics, such as tiotropium or β-agonists, such as Albuterol.
- Continuous positive airway pressure (CPAP).
- Inhaled steroid medications to decrease inflammation.
- Lung transplant, in rare cases.
- Mechanical ventilation, if oxygen therapy is not sufficient to increase blood oxygen levels.
- Oxygen therapy to increase blood oxygen levels.
- Tracheostomy, a hole made in the front of the neck to help breathing.
- A patient whose breathing remains very poor will require a ventilator to aid breathing.
- Suctioning the lungs through a small plastic tube passed through the nose, in order to remove secretions from the airways that the patient cannot cough up.